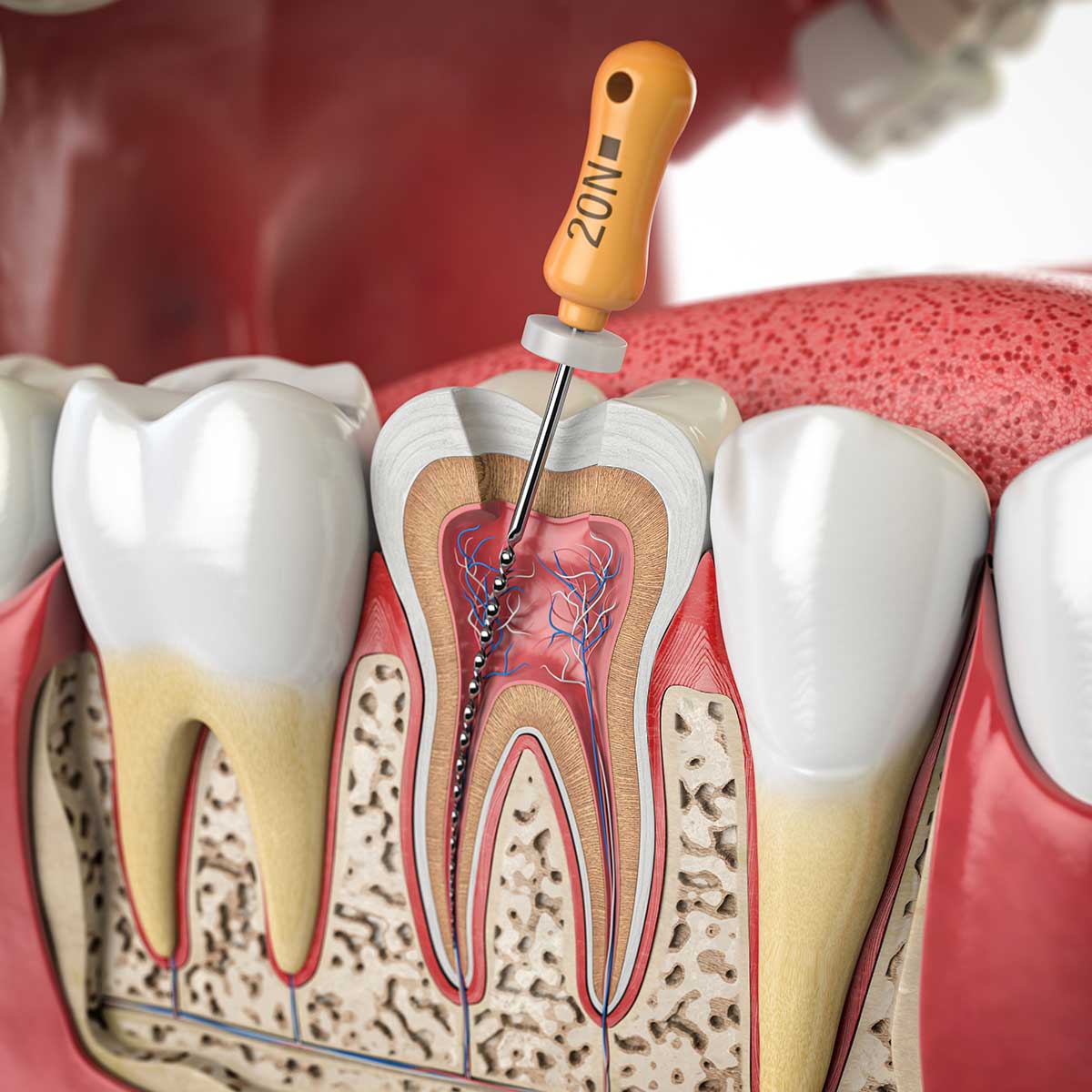
What is a Root Canal?
Teeth are made up of three layers:
- Enamel
- Dentin
- Cementum
There is a space inside the hard layer of each tooth. It is called the root canal system and it is filled with soft dental pulp. This pulp is made up of nerves and blood vessels that help the tooth grow and develop. Once a tooth is fully grown, it can survive without a pulp. If the pulp of the tooth becomes infected, then a root canal (or endodontic treatment) is needed. When this is done, the pulp is removed.
When is a Root Canal Needed?
The pulp inside the tooth can be damaged by cracks in the tooth, deep cavities, old fillings that leak and allow bacteria underneath them or trauma due to accidents. Germs (or bacteria) can get into the tooth and can lead to an infected tooth pulp. This may cause pain and/or swelling. Sometimes a pulp becomes infected or dies, but does not cause any pain. Your dentist may notice:
- Changes in the colour of your tooth
- Change in your gums or
- Changes picked up by a dental x-ray
Sometimes, if a great deal of dental work is needed, your dentist can tell you from an examination and an x-ray that the pulp of the tooth is most likely not going to survive and a root canal treatment may be necessary.
Dentists and Root Canals
During your regular check-up your dentist checks for infection and damage to teeth even though you may not notice any signs of tooth trouble. If trouble is spotted and you need a root canal your dentist may do it, or refer you to a specialist. Root canal specialists are called Endodontists. If you notice a problem with a tooth do NOT wait until it hurts. Call your dentist as soon as you notice a cavity or loose filling, or as soon as a tooth is injured. If you get attention quickly there is a better chance that damage can be prevented and that the tooth can be saved.
If you have noticed a change in your teeth or experienced pain, contact us today.
How Is a Root Canal Procedure Done?
Step 1: Evaluation & Appointment Planning
A root canal can sometimes be completed in a single visit, while more complex cases may require multiple appointments. This depends on the shape of the root canal system and the extent of pulp damage or infection. If the infection has spread to the surrounding bone or formed an abscess, it may need to be drained before the tooth can be fully treated.
Step 2: Tooth Isolation
A member of the dental team places a rubber dam around the affected tooth. This keeps the area clean and dry, protects the tooth from saliva and bacteria, and prevents you from swallowing any materials used during the procedure.
Step 3: Anesthesia (If Needed)
Dr. Inigo may administer local anesthetic (“freezing”) to ensure comfort during the procedure. In some cases, anesthesia may not be necessary.
Step 4: Accessing the Tooth
A small opening is made in the tooth to reach the root canal system and the damaged or infected pulp inside.
Step 5: Cleaning the Root Canals
The infected pulp is carefully removed. Using very fine dental instruments, the root canals are cleaned, shaped, and enlarged to eliminate bacteria and prepare them for filling.
Step 6: Filling and Sealing
Once thoroughly cleaned, the root canals are filled and sealed with a rubber-like material called gutta-percha to prevent reinfection.
Step 7: Restoring the Tooth
The tooth is sealed with either a temporary or permanent filling. In many cases, a crown may be recommended later to restore strength and protect the treated tooth.
Aftercare, Restoration & Long-Term Tooth Health
Don’t Let Tooth Pain Get Worse
If you’re experiencing tooth pain or have been told you need a root canal, early treatment can make all the difference. Our team is committed to providing gentle, effective care to help you save your natural tooth and restore your comfort. Contact us today and book your appointment and take the next step toward a healthier, pain-free smile.


